Lymphatic filariasis is one of the world’s leading causes of permanent and long-term disability. Sometimes referred to as Elephantiasis tropica, it is a neglected and stigmatised mosquito-borne disease. It damages the human lymphatic system, leading to disfiguring swelling of limbs, breasts and genitals.
How do people get lymphatic filariasis?
People are primarily infected with the disease through mosquito bites. In Africa, the Anopheles mosquito is the main vector. The female Anopheles mosquito transmits microscopic filarial parasitic worms (Wuchereria bancrofti, Brugia timori and Brugia malayi) from one person to another during its feeding process. These worms then live and grow in the human lymphatic system, causing disruption and damage. The lymphatic system is part of the immune system – it works primarily to maintain the body fluid levels and protects the body from pathogens.
The primary method of prevention is to avoid being bitten by mosquitoes in endemic areas. The disease is common in tropical regions of the world, where water collects outdoors and there are poor sanitary conditions. Infection takes more than one bite – those most at risk are people who are bitten repeatedly over time. Research in Ghana, for example, shows that risk factors include a mixture of environmental and economic conditions. These include proximity to the coast or short savanna grass areas, rainfall and temperature, season, and poverty and poor housing.
What is it like to live with lymphatic filariasis?
People with lymphatic filariasis experience acute filarial attacks. Filarial attacks involve a fever, and swelling and peeling skin on the affected areas of the body. The causes of the attacks are believed to include microbial contamination and immune reactions to the presence of the live or dead adult worms. The main visible sign of the illness is disfiguring swelling, followed by peeling of the affected area. In women this swelling, called lymphedema or elephantiasis, mainly affects arms and legs. In men it can also cause enlargement of the scrotum, referred to as hydrocele.
The swelling affects people’s lives in a multitude of ways. It can interfere with the fit of clothing and shoes, impair mobility, and affect sexual function. The harm is more than physical. It can also result in serious economic, social and interpersonal consequences.
As a former UN Special Rapporteur on the Right to Health, Paul Hunt, has argued:
the human rights implications of neglected diseases have not been given the attention they deserve.
Due to a combination of disability, stigma and discrimination, people with lymphatic filariasis often lose their jobs, are shunned from their communities and have difficulty starting or maintaining relationships. The stigma, ill-treatment and isolation that results from this condition can, in turn, lead to negative mental health outcomes.
How is it being addressed?
Lymphatic filariasis cannot be cured. However, recent studies show tetracycline-based antibiotics could be helpful, particularly in the early stages. Given the issue of multidrug resistance to antibiotics, however, this is not normally encouraged on a large scale.
The Global Programme for Elimination of Lymphatic Filariasis aims to interrupt the transmission of the infection and manage the conditions that accompany it by mass drug administration in endemic communities. The programme has achieved some notable successes, but it continues to face challenges. Despite more than a decade of work, lymphatic filariasis remains endemic in 31 African countries.
Public awareness campaigns and strict adherence to mass drug administration campaigns are important tools of prevention and eradication. It is also necessary to ensure the clearing of bushes, dredging of choked gutters, and proper disposal of refuse in endemic communities to interrupt mosquito breeding sites.
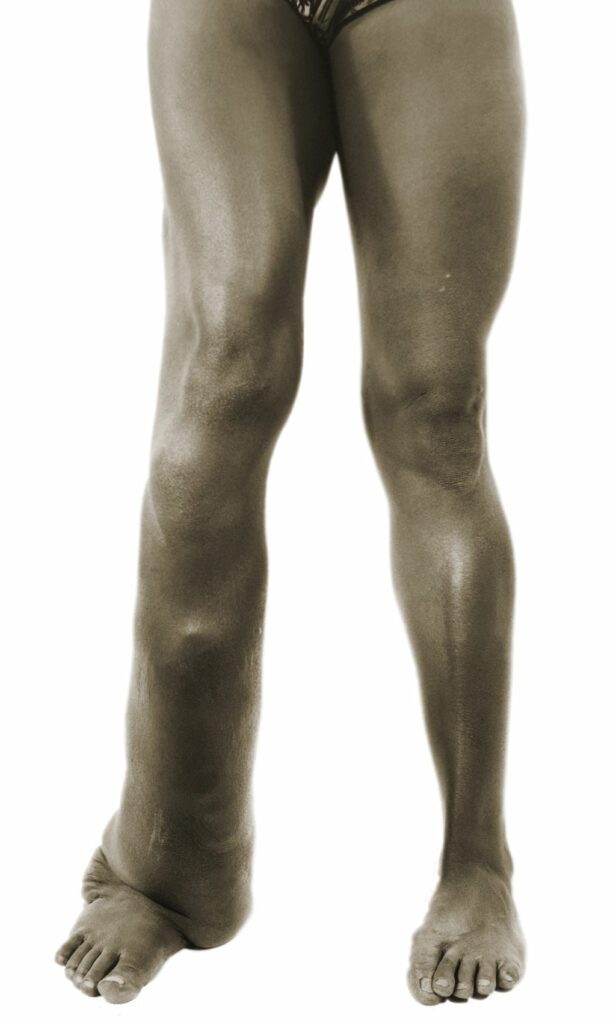
Credit: CDC / Robert S. Craig
What are the barriers to eradicating it?
Barriers to eradication are not straightforward. Research and interventions have been overwhelmingly biomedical, focusing largely on mass drug administration (ivermectin, albendazole, diethycarbarmazine). Drugs work by killing the larval stages of the parasites. They have little effect on the adult worms, so they need to be given yearly. However, these drugs can only save a person from disfigurement if they are taken early and regularly.
Placing the illness in the context of the local culture is still a major challenge for health practitioners. The lack of cultural engagement in eradication programmes is in itself a barrier. People with lymphatic filariasis view the illness through their cultural traditions. Often they blame outside invisible forces such as witchcraft, sorcery or ancestral curses when they contract the disease. Logically, they may spend as much time seeking help from ritualists and priests to fight off these dangerous spirits as they might spend following a western medical regimen. They may understand healing the spiritual and social self to be as important as healing the bodily self.
Gender dynamics can also be an important factor in seeking treatment. Women may face social and financial barriers in accessing treatment.
ABOUT THE AUTHORS
Alexander Kwarteng, Lecturer in Immunology of Infectious Diseases, Kwame Nkrumah University of Science and Technology (KNUST). My background is in Molecular Biomedicine and I have invested several years of research in host-pathogen interaction. In addition to this, I have been involved in a number of studies that focus on the microbiome in parasite infections in Ghana. However, the increasing prevalence of infectious diseases in Ghana and other African countries ignited my passion to focus on the use of bioinformatics tools to understand underlying genomic and immunology presentations of diseases and other medical conditions, as well as the use of social determinants to understand how people perceive the disease. I am excited to contribute to the training of postgraduates and postdoctoral fellows in the proposed program. He is an expert in infectious disease and has established several collaborations with renowned scientists in many parts of the world.
Jonathan Roberts, Associate Professor, Mount Saint Vincent University. Roberts is a specialist in the history of medicine and religion in West Africa. His recent book, Sharing the Burden: A History of Healing in Accra, is the culmination of years of archival and interview research in the capital of Ghana. Roberts asserts that a commitment to pluralism, rather than a singular medical tradition, allowed several forms of a healing to flourish in Accra. This meant that Western medicine, rather than triumphing as the dominant healing paradigm, became only one of many options for patients and their caregivers. This focus on pluralism guides his current project: A History of Western Medicine in Africa. Jonathan has also written about the history of pandemics, teaches a course at the Mount called Plagues and Peoples, and has offered public commentary on outbreaks of Ebola, influenza and the coronavirus. He advocates for transparency and openness during pandemics, as a way to avoid the scapegoating and conspiracy theories that have been prevalent during past outbreaks.
Kristi Heather Kenyon, Associate Professor, University of Winnipeg. Kristi Heather Kenyon is an Associate Professor in the Human Rights program at the University of Winnipeg’s Global College. With an emphasis on sub-Saharan Africa, her research focuses on health and human rights, examining how and why civil society groups mobilize on stigmatized conditions and populations, and how health and human rights are understood in social and cultural context. Her 2017 book Resilience and Contagion: Invoking Human Rights in African HIV Advocacy (McGill-Queens University Press) interrogates why, when and how NGOS use human rights in HIV advocacy. Prior to her current appointment, she held a SSHRC postdoctoral fellowship at Dalhousie University and a Centre for Human Rights postdoctoral fellowship at the University of Pretoria. She completed her PhD in Political Science at the University of British Columbia supported by the Trudeau Foundation and SSHRC. Her research is informed by more than 15 years of work in, with and on civil society, including work as a human rights practitioner in Southern Africa and Southeast Asia and service on the board of local and international development organizations in Canada and Botswana. She was a 2017-2019 CIFAR-Azrieli Global Scholar with the Canadian Institute for Advanced Research, and is a Research Fellow with the Centre for the Study of Security and Development at Dalhousie University.
Mary Asirifi is an Assistant Professor, at the Faculty of Nursing, Department of Nursing Foundations in MacEwan University. Mary joined MacEwan University in 2017 and is currently teaching undergraduate nursing courses. While Mary is originally from Ghana, where she completed her diploma and baccalaureate nursing education, her MN and PhD degrees are from the Faculty of Nursing at the University of Alberta. Mary achieved nurse registration with the College & Association of Registered Nurses of Alberta (CARNA) in Canada in 2013. She has clinical experience in medical-surgical nursing as a registered nurse in both Ghana and Alberta. Mary was a nurse tutor in Ghana.
This article is courtesy of The Conversation.


