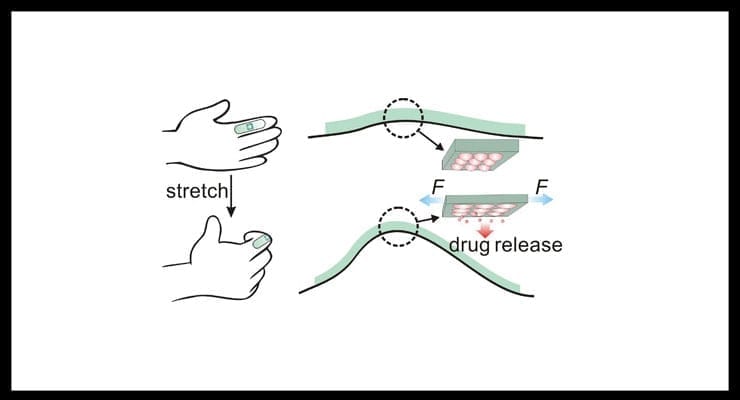
Researchers from North Carolina State University and the University of North Carolina at Chapel Hill have developed a drug delivery technology that consists of an elastic patch that can be applied to the skin and will release drugs whenever the patch is stretched.
For example, if applied to the elbow, the patch would release a drug when the elbow bends and stretches the patch.
“This could be used to release painkillers whenever a patient with arthritic knees goes for a walk, or to release antibacterial drugs gradually as people move around over the course of a day,” says Zhen Gu, co-senior author of a paper describing the work and an assistant professor in the joint biomedical engineering program at NC State and UNC-Chapel Hill.
The technology consists of an elastic film that is studded with biocompatible microcapsules. These microcapsules, in turn, are packed with nanoparticles that can be filled with drugs.
Here’s how it works: The microcapsules stick halfway out of the film, on the side of the film that touches a patient’s skin. The drugs leak slowly out of the nanoparticles and are stored in the microcapsules. When the elastic film is stretched, it also stretches the microcapsules – enlarging the surface area of the microcapsule and effectively squeezing some of the stored drug out onto the patient’s skin, where it can be absorbed.
“When the microcapsule is stretched from left to right, it is also compressed from bottom to top,” says Yong Zhu, co-senior author of the paper and an associate professor of mechanical and aerospace engineering at NC State. “That compression helps push the drug out of the microcapsule.”
After being stretched, the microcapsule is “re-charged” by the drugs that continue to leak out of the nanoparticles.
“This can be used to apply drugs directly to sites on the skin, such as applying anti-cancer medications to melanomas or applying growth factors and antibiotics for wound healing,” says Jin Di, co-lead author and a Ph.D student in Gu’s lab.
The researchers also incorporated microneedles into the system, applying them on top of the microcapsules. In this configuration, the drugs can be squeezed through the microneedles. The microneedles are small enough to be painless, but large enough to allow drugs to diffuse into the bloodstream through tiny capillaries underneath the skin. “This expands the range of drugs that can be applied using the technology,” says Shanshan Yao, co-lead author and a Ph.D student in Zhu’s lab.
“We’re now exploring how this tool can be used to apply drugs efficiently and effectively to burn patients, and we plan to look at how this could be used for pain relief as well,” Gu says.
“The materials are relatively inexpensive, and the manufacturing process is fairly straightforward, so we’re optimistic that this could be scaled up in a cost-effective way,” Zhu says.
Read more: Stretch-Triggered Drug Delivery from Wearable Elastomers Containing Therapeutic Depots.