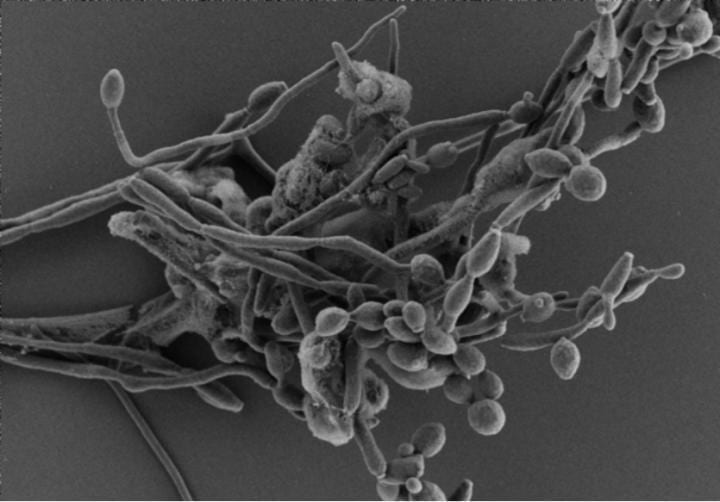
Researchers from Umeå University have shown how adaption of microbial fungi to low oxygen environments influences their recognition by immune cells and their ability to thrive and cause harmful infection within the host.
The research was published recently in the journal mBio, a publication of the American Society of Microbiology.
“It was very surprising to see that the fungus does not require oxygen to cause disease. Unexpectedly, the microbial pathogen could even use low oxygen environments to evade immune attack and to become more virulent.” – says Constantin Urban, Associated Professor at the Department of Clinical Microbiology.
Interestingly, C. albicans is a commensal microbe of our gastrointestinal system and when natural barriers fail, due to immunosuppressive disease or treatment, C. albicans can spread from its natural reservoir and invade the body to cause life-threatening, systemic disease. “We now understand how C. albicans under these circumstances exploits the training from anoxic commensal niches to thrive in deep-seeded body sites which quickly induce inflammation and immune cell recruitment. Both processes rapidly exhaust oxygen and in turn create low oxygen milieus.” – continues Dr. Urban.
Candida albicans is the most common fungal pathogen and a common cause of sepsis. While most individuals are infected with Candida albicans since birth, the infection causes serious illness or even death, particularly among those with a weakened immune system. Their new study is a step towards the characterization of immune responses under low oxygen levels, a frequent stress condition during inflammation and infection. Particularly neutrophils, the most abundant white blood cell and essential defence line against fungal microbes, where hampered in their ability to attack and eradicate C. albicans under low oxygen conditions, whereas the neutrophils’ metabolism and viability seemed unaffected.
The research may be applied to future therapy strategies to reduce premature deaths and to improve patients’ life quality.