Using a novel statistical model, a research team led by Columbia University’s Mailman School of Public Health mapped the spread of the 2014-2015 Ebola outbreak in Sierra Leone, providing the most detailed picture to date on how and where the disease spread and identifying two critical opportunities to control the epidemic.
The result, published in the Journal of the Royal Society Interface, matches with details known about the early phase of the Ebola outbreak, suggesting the real-time value of the method to health authorities as they plan interventions to contain future outbreaks, and not just of Ebola.
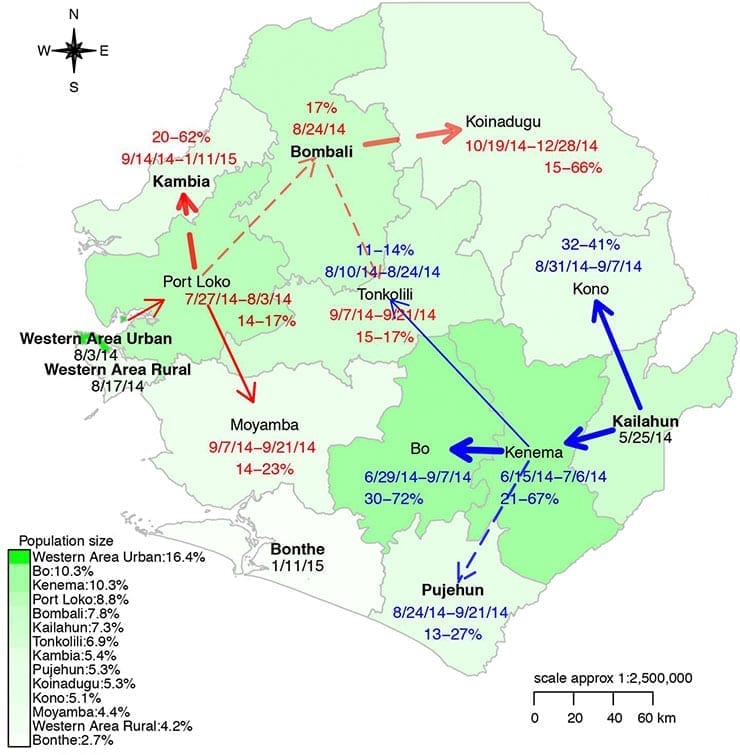
Their analysis uses data from the Sierra Leone Ministry of Health and Sanitation to chart the course of the Ebola outbreak, beginning with the arrival of the disease in the border district of Kailahun in late May 2014.
By mid-June, Ebola spread west to nearby Kenema–a pathway consistent with a recent field investigation. At its peak, 67 percent of Ebola cases in Kenema were imported from Kailahun; by early July, the epidemic was firmly established in Kenema with most cases infected locally. From Kenema, the outbreak continued west, south, and north. Beginning in early July, a second path emerged in capital city, Freetown, spreading east to Port Loko by late July, then quickly east and south.
Because of their many connections to other districts, Kenema and Port Loko were critical junction points for the outbreak. At these points, windows of opportunity may have existed for controlling the spread of Ebola within Sierra Leone, the study suggests. The researchers estimate that first window, before Ebola reached Kenema, was approximately one month. The second window, before it reached Port Loko, was much shorter.
The method described in the paper uses three principal ingredients: the home district of the Ebola-positive patient, the population of that district, and geographic distance between districts–all information that was available during the outbreak.
“While this analysis is too late to be used for application to and intervention in the Ebola epidemic, the method we used could be useful for future disease outbreaks, and not just for Ebola,” says Jeffrey Shaman, PhD, the study’s senior author and associate professor of Environmental Health Sciences at the Mailman School.
“To be able to infer the spatial-temporal course of an outbreak and the rate of its spread between population centers in real time,” Shaman continues, “may greatly aid public health planning, including the level and speed of deployment of intervention measures such as how many doctors and beds are needed and where to put them.”
The traditional method to track disease spread is contract tracing, in which health workers interview patients and everyone they came into contact with. “Contact tracing is highly labor intensive,” says lead author Wan Yang, PhD, associate research scientist at the Mailman School. “Especially in resource-poor areas, an epidemic like Ebola can easily outrun any such effort to track it. The minimal information needed in our method makes it a particularly valuable tool to aid public health efforts during a novel disease outbreak in these areas.”
During the Ebola outbreak, there was a collapse of the healthcare system in Sierra Leone. Observational data were very limited and error-laden. “Having the ability to infer the course of the outbreak gives officials the ability to see what’s happening rather than flying completely blind,” Shaman says. “In a public health emergency, it’s critical that they have as much information as possible so they can make informed decisions.
“If you had perfect observation,” Shaman adds, “you wouldn’t need these methods, but you’re never going to get that.”
Previous work by Shaman and Yang has used computational methods to predict infectious disease spread. Beginning in the summer of 2014, they generated weekly estimates of countrywide Ebola incidence in Sierra Leone, Guinea, and Liberia. They also developed a prize-winning method to forecast seasonal influenza. Forecasts are available online at Columbia Prediction of Infectious Diseases.
The study was supported by grants from the National Institutes of Health and the Research and Policy for Infectious Disease Dynamics (RAPIDD) program of the Department of Homeland Security.
Read the study: Transmission network of the 2014–2015 Ebola epidemic in Sierra Leone. DOI: 10.1098/rsif.2015.0536

