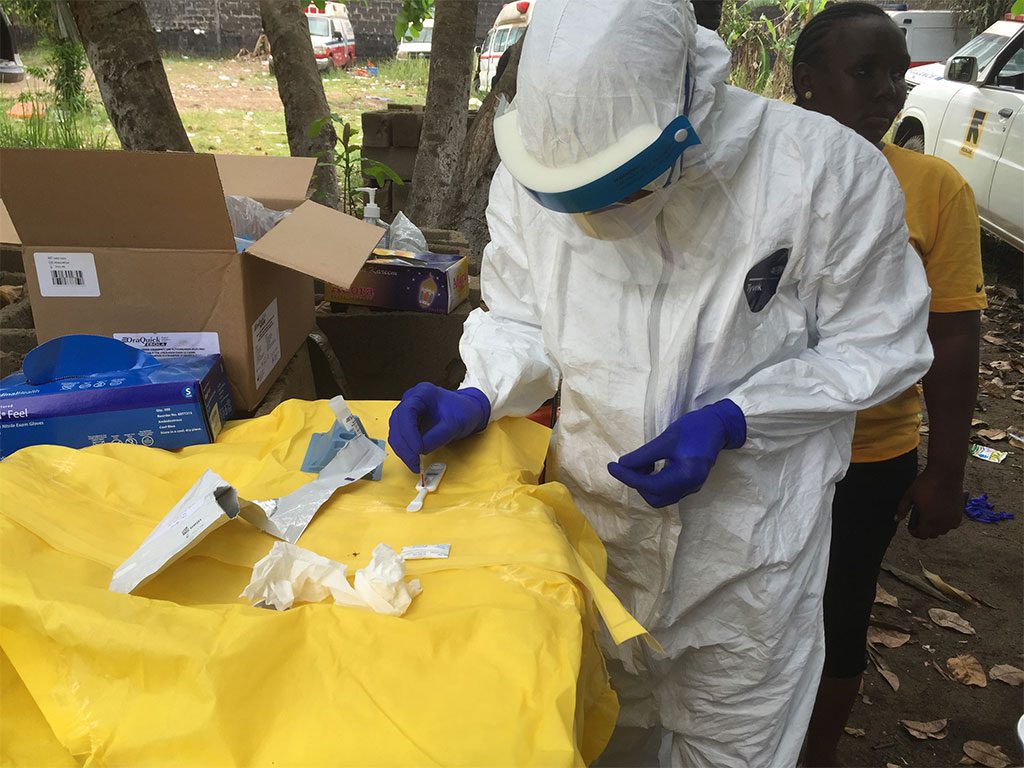
More than 300 suspected cases and at least 80 deaths into an accelerating outbreak, the World Health Organization declared the Ebola epidemic spreading across the Democratic Republic of the Congo and Uganda a public health emergency of international concern (PHEIC) on Sunday, May 17, 2026. The declaration, the most serious alarm WHO can raise short of a pandemic emergency, reflects both the scale of what is already visible and deep uncertainty about how much more may be going undetected in one of the world’s most conflict-affected and logistically challenging regions.
The outbreak is caused by the Bundibugyo virus, a strain of Ebola that is less commonly encountered than the Zaire strain responsible for most of the DRC’s 17 previous outbreaks. Unlike Zaire-strain Ebola, for which approved vaccines and therapeutics now exist, no licensed countermeasures are currently available for Bundibugyo virus disease. WHO described this gap as a key reason the event qualifies as extraordinary under the terms of the International Health Regulations.
What the Numbers Show — and What They May Be Missing
As of May 16, WHO reported eight laboratory-confirmed cases, 246 suspected cases, and 80 suspected deaths in Ituri Province in eastern DRC, spread across at least three health zones: Bunia, Rwampara, and Mongbwalu. The Africa CDC reported 336 suspected cases and 87 deaths by May 17, and updated figures from the AP placed the total at 88 deaths at the time of the PHEIC declaration.
Those numbers may significantly undercount the true scope of the outbreak. WHO noted that eight of the first 13 samples collected across various areas tested positive — a high positivity rate that suggests widespread circulation. The agency warned that the combination of increasing syndromic reporting, clusters of unexplained community deaths, and confirmed spread to both Kinshasa and Kampala points toward a potentially much larger outbreak than what surveillance is currently capturing.
International Spread Already Documented
The geographic reach of the outbreak has grown rapidly. On May 15 and 16, two laboratory-confirmed cases — apparently unrelated to each other — were reported in Kampala, Uganda, both among individuals who had traveled from the DRC. One of those patients died. Both were admitted to intensive care units in the Ugandan capital. A third laboratory-confirmed case was reported in Kinshasa, the DRC’s capital, in a person who had returned from Ituri. Ituri Province lies roughly 1,000 kilometers from Kinshasa, and the confirmation of a case there underscores the mobility driving the outbreak’s spread.
Africa CDC Director-General Dr. Jean Kaseya, speaking at an online briefing, noted that the outbreak originated in the Mongwalu health zone, a high-traffic mining area, and subsequently spread to Rwampara and Bunia as patients traveled seeking care. A high number of active cases remain in the community, particularly in Mongwalu, he said, significantly complicating containment and contact tracing.
A Perfect Storm of Risk Factors
Eastern DRC presents some of the most difficult conditions imaginable for outbreak response. Ituri Province has been under sustained attack from Islamic State-affiliated militants, restricting the movement of health workers and supplies and limiting surveillance capacity. The informal health system — characterized by a large network of unlicensed and loosely regulated facilities — creates additional opportunities for healthcare-associated transmission. WHO reported that at least four healthcare workers have already died in circumstances consistent with viral hemorrhagic fever, raising concerns about infection prevention and control gaps within health facilities. Residents of Bunia described daily burials in interviews with Associated Press journalists on the ground.
The combination of active conflict, high population mobility, urban transmission in Bunia and Kinshasa, and the absence of approved medical countermeasures led WHO to characterize the situation as carrying significant local and regional risk of spread — comparable in some respects to the 2018-2019 North Kivu and Ituri epidemic, which ultimately infected more than 3,000 people.
WHO’s Guidance: Isolate, Screen, Do Not Close Borders
In issuing the PHEIC, WHO Director-General Tedros Adhanom Ghebreyesus offered a range of guidance to affected and neighboring countries. For the DRC and Uganda, the agency called for activation of national emergency operations centers, strengthened surveillance and contact tracing, decentralized laboratory capacity, and dedicated isolation and treatment facilities near outbreak epicenters. WHO urged immediate exit screening at international airports, seaports, and major land crossings, and specified that confirmed cases should not travel nationally or internationally until two virus-specific diagnostic tests conducted at least 48 hours apart return negative results. Contacts should be monitored daily and barred from international travel for 21 days after exposure.
For countries sharing land borders with the DRC, WHO called for urgent enhancement of preparedness, including active surveillance, rapid response teams, and access to qualified diagnostic laboratories. For all other countries, the agency was explicit: no nation should close its borders or restrict trade. Such measures, WHO stated, are not grounded in science, tend to push movement toward unmonitored informal crossings, and risk undermining both response logistics and local economies.
Emergency Mobilization
The Bundibugyo strain’s emergence as the cause of the DRC’s 17th Ebola outbreak since 1976 represents a distinct and underappreciated threat. While the global health community has invested heavily in Zaire-strain countermeasures following the West Africa epidemic of 2014-2016 and the North Kivu epidemic of 2018-2019, Bundibugyo remains without approved vaccines or treatments, leaving response teams dependent entirely on supportive care, isolation, and contact tracing. The strain has caused outbreaks before — most notably in Uganda in 2007 — but has received far less countermeasure development attention.
The PHEIC designation is intended to trigger international coordination and resource mobilization. WHO announced it will convene an Emergency Committee as soon as possible to advise on temporary recommendations. Whether the international community can mount a rapid and effective response in an active conflict zone, with no licensed medical tools and a likely undercounted case burden, will define how far this outbreak spreads.
Sources and further reading:
WHO declares Ebola outbreak in Congo and Uganda ’emergency’ of international concern – The Guardian
WHO declares global health emergency over Ebola outbreak in Congo and Uganda – AP
WHO declares Ebola outbreak in Congo, Uganda an emergency of international concern – Reuters